Introduction
Vitamin D is traditionally associated with bone health, yet growing scientific evidence shows that it functions more like a hormone than a conventional vitamin. It plays a crucial role in endocrine signaling, calcium metabolism, reproductive health, and metabolic regulation. Maintaining adequate vitamin D levels is therefore essential for sustaining hormonal balance and overall physiological stability.
Vitamin D as a Hormone: A Unique Biological Messenger
Unlike most vitamins, vitamin D can be synthesized in the human body and converted into an active hormonal form. Once activated, it binds to vitamin D receptors (VDRs) present in multiple tissues including the brain, thyroid, pancreas, ovaries, and immune cells.
Key Hormonal Functions
- Regulates gene expression involved in hormone production
- Influences cellular communication between endocrine glands
- Supports inflammatory balance affecting hormonal signaling
Research suggests that vitamin D acts similarly to steroid hormones by influencing transcriptional activity and metabolic pathways (source). This widespread receptor distribution explains why deficiency may contribute to hormonal dysregulation and systemic symptoms.
How Vitamin D Is Produced and Activated in the Body
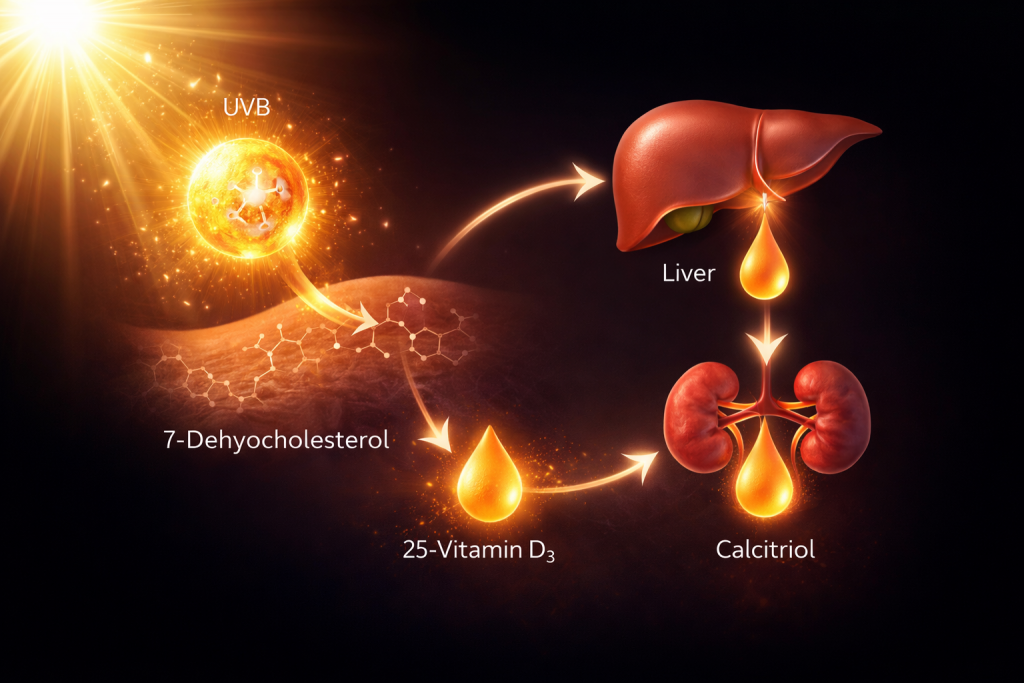
Vitamin D synthesis begins when ultraviolet B (UVB) radiation from sunlight converts 7-dehydrocholesterol in the skin into pre-vitamin D₃. This compound is transported to the liver and converted into 25-hydroxyvitamin D, the main circulating form. A second activation step occurs in the kidneys, producing calcitriol — the biologically active hormone.
Sources of Vitamin D
- Sunlight exposure
- Dietary intake (fatty fish, fortified foods, egg yolks)
- Nutritional supplementation
Factors such as aging, limited sun exposure, skin pigmentation and gastrointestinal disorders can impair this synthesis pathway. Reduced activation may consequently influence endocrine responsiveness and hormonal equilibrium.
Role of Vitamin D
One of vitamin D’s most critical physiological roles is enhancing calcium absorption in the intestines. It stimulates the production of calcium-binding proteins that facilitate mineral transport into the bloodstream.
How Vitamin D Supports Calcium Uptake
- Increases expression of calcium transport channels
- Promotes intestinal calcium-binding protein synthesis
- Maintains serum calcium levels required for hormonal secretion
Stable calcium signaling is essential for endocrine gland activity. Hormones such as insulin and parathyroid hormone depend on calcium-mediated cellular processes. According to research, vitamin D deficiency reduces calcium absorption efficiency, potentially disrupting metabolic and hormonal balance (source).
Hormones Influenced by Vitamin D
Vitamin D affects multiple hormone systems that regulate reproduction, metabolism, and mood.
Estrogen and Reproductive Hormones
Vitamin D receptors in ovarian tissue suggest a role in follicular development and estrogen synthesis. Lower vitamin D levels have been associated with menstrual irregularities and reproductive disorders such as Polycystic Ovary Syndrome.
Insulin and Metabolic Hormones
Vitamin D may enhance insulin sensitivity by improving pancreatic beta-cell function and reducing inflammation. This effect can help stabilize blood glucose levels and reduce metabolic stress.
Thyroid Hormone Activity
Emerging studies indicate that vitamin D influences thyroid autoimmunity and hormone regulation, although mechanisms are still being explored.
Hormonal Imbalance Linked to Low Vitamin D
Vitamin D deficiency can contribute to symptoms commonly linked with endocrine disruption.
Common Indicators
- Persistent fatigue or low energy
- Mood fluctuations and increased stress sensitivity
- Hair thinning or slow hair growth
- Irregular menstrual cycles
- Reduced bone density or muscle weakness
Because vitamin D impacts both calcium metabolism and hormone receptor activity, long-term deficiency may gradually impair physiological resilience. Blood testing and timely nutritional intervention can help restore balance and prevent complications.
How Much Vitamin D Is Needed for Hormone Health?
Optimal vitamin D intake varies depending on individual health status, lifestyle, and geographic factors. Many health authorities recommend 600–800 IU daily for adults, although higher doses may be required in cases of deficiency under medical supervision.
Practical Hormone-Support Strategies
- Safe sunlight exposure for natural synthesis
- Balanced diet rich in vitamin D and calcium
- Personalized supplementation when necessary
- Regular monitoring of serum vitamin D levels
Vitamin D works together with calcium; therefore, ensuring adequate mineral intake supports endocrine function and skeletal integrity. Excessive supplementation should be avoided to prevent toxicity and metabolic imbalance.
Conclusion
Vitamin D plays a varied role in hormonal balance by functioning as a hormone itself, enhancing calcium absorption, and influencing endocrine signaling pathways. Its effects on reproductive hormones, insulin sensitivity, thyroid function, and immune regulation highlight its importance in maintaining systemic stability. Supporting healthy vitamin D levels through sunlight, nutrition, and responsible supplementation can promote hormonal harmony, improved energy levels, and long-term wellness.


